18.2: Cold and Allergy Medicines
- Page ID
- 156210
\( \newcommand{\vecs}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vecd}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash {#1}}} \)
\( \newcommand{\id}{\mathrm{id}}\) \( \newcommand{\Span}{\mathrm{span}}\)
( \newcommand{\kernel}{\mathrm{null}\,}\) \( \newcommand{\range}{\mathrm{range}\,}\)
\( \newcommand{\RealPart}{\mathrm{Re}}\) \( \newcommand{\ImaginaryPart}{\mathrm{Im}}\)
\( \newcommand{\Argument}{\mathrm{Arg}}\) \( \newcommand{\norm}[1]{\| #1 \|}\)
\( \newcommand{\inner}[2]{\langle #1, #2 \rangle}\)
\( \newcommand{\Span}{\mathrm{span}}\)
\( \newcommand{\id}{\mathrm{id}}\)
\( \newcommand{\Span}{\mathrm{span}}\)
\( \newcommand{\kernel}{\mathrm{null}\,}\)
\( \newcommand{\range}{\mathrm{range}\,}\)
\( \newcommand{\RealPart}{\mathrm{Re}}\)
\( \newcommand{\ImaginaryPart}{\mathrm{Im}}\)
\( \newcommand{\Argument}{\mathrm{Arg}}\)
\( \newcommand{\norm}[1]{\| #1 \|}\)
\( \newcommand{\inner}[2]{\langle #1, #2 \rangle}\)
\( \newcommand{\Span}{\mathrm{span}}\) \( \newcommand{\AA}{\unicode[.8,0]{x212B}}\)
\( \newcommand{\vectorA}[1]{\vec{#1}} % arrow\)
\( \newcommand{\vectorAt}[1]{\vec{\text{#1}}} % arrow\)
\( \newcommand{\vectorB}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vectorC}[1]{\textbf{#1}} \)
\( \newcommand{\vectorD}[1]{\overrightarrow{#1}} \)
\( \newcommand{\vectorDt}[1]{\overrightarrow{\text{#1}}} \)
\( \newcommand{\vectE}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash{\mathbf {#1}}}} \)
\( \newcommand{\vecs}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vecd}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash {#1}}} \)
\(\newcommand{\avec}{\mathbf a}\) \(\newcommand{\bvec}{\mathbf b}\) \(\newcommand{\cvec}{\mathbf c}\) \(\newcommand{\dvec}{\mathbf d}\) \(\newcommand{\dtil}{\widetilde{\mathbf d}}\) \(\newcommand{\evec}{\mathbf e}\) \(\newcommand{\fvec}{\mathbf f}\) \(\newcommand{\nvec}{\mathbf n}\) \(\newcommand{\pvec}{\mathbf p}\) \(\newcommand{\qvec}{\mathbf q}\) \(\newcommand{\svec}{\mathbf s}\) \(\newcommand{\tvec}{\mathbf t}\) \(\newcommand{\uvec}{\mathbf u}\) \(\newcommand{\vvec}{\mathbf v}\) \(\newcommand{\wvec}{\mathbf w}\) \(\newcommand{\xvec}{\mathbf x}\) \(\newcommand{\yvec}{\mathbf y}\) \(\newcommand{\zvec}{\mathbf z}\) \(\newcommand{\rvec}{\mathbf r}\) \(\newcommand{\mvec}{\mathbf m}\) \(\newcommand{\zerovec}{\mathbf 0}\) \(\newcommand{\onevec}{\mathbf 1}\) \(\newcommand{\real}{\mathbb R}\) \(\newcommand{\twovec}[2]{\left[\begin{array}{r}#1 \\ #2 \end{array}\right]}\) \(\newcommand{\ctwovec}[2]{\left[\begin{array}{c}#1 \\ #2 \end{array}\right]}\) \(\newcommand{\threevec}[3]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \end{array}\right]}\) \(\newcommand{\cthreevec}[3]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \end{array}\right]}\) \(\newcommand{\fourvec}[4]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \\ #4 \end{array}\right]}\) \(\newcommand{\cfourvec}[4]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \\ #4 \end{array}\right]}\) \(\newcommand{\fivevec}[5]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \\ #4 \\ #5 \\ \end{array}\right]}\) \(\newcommand{\cfivevec}[5]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \\ #4 \\ #5 \\ \end{array}\right]}\) \(\newcommand{\mattwo}[4]{\left[\begin{array}{rr}#1 \amp #2 \\ #3 \amp #4 \\ \end{array}\right]}\) \(\newcommand{\laspan}[1]{\text{Span}\{#1\}}\) \(\newcommand{\bcal}{\cal B}\) \(\newcommand{\ccal}{\cal C}\) \(\newcommand{\scal}{\cal S}\) \(\newcommand{\wcal}{\cal W}\) \(\newcommand{\ecal}{\cal E}\) \(\newcommand{\coords}[2]{\left\{#1\right\}_{#2}}\) \(\newcommand{\gray}[1]{\color{gray}{#1}}\) \(\newcommand{\lgray}[1]{\color{lightgray}{#1}}\) \(\newcommand{\rank}{\operatorname{rank}}\) \(\newcommand{\row}{\text{Row}}\) \(\newcommand{\col}{\text{Col}}\) \(\renewcommand{\row}{\text{Row}}\) \(\newcommand{\nul}{\text{Nul}}\) \(\newcommand{\var}{\text{Var}}\) \(\newcommand{\corr}{\text{corr}}\) \(\newcommand{\len}[1]{\left|#1\right|}\) \(\newcommand{\bbar}{\overline{\bvec}}\) \(\newcommand{\bhat}{\widehat{\bvec}}\) \(\newcommand{\bperp}{\bvec^\perp}\) \(\newcommand{\xhat}{\widehat{\xvec}}\) \(\newcommand{\vhat}{\widehat{\vvec}}\) \(\newcommand{\uhat}{\widehat{\uvec}}\) \(\newcommand{\what}{\widehat{\wvec}}\) \(\newcommand{\Sighat}{\widehat{\Sigma}}\) \(\newcommand{\lt}{<}\) \(\newcommand{\gt}{>}\) \(\newcommand{\amp}{&}\) \(\definecolor{fillinmathshade}{gray}{0.9}\)- Know the cause of the common cold and allergies.
- Know the chemical name, common name, and uses of different cough, cold, and allergy medicines.
The common cold is a viral infectious disease of the upper respiratory tract which affects primarily the nose. The symptoms of the common cold are believed to be primarily related to the immune response to the virus. Symptoms include coughing, sore throat, runny nose, and fever which usually resolve in seven to ten days, with some symptoms lasting up to three weeks. Well over 200 viruses are implicated in the cause of the common cold. The most commonly implicated virus is a rhinovirus (30–80%).
No cure for the common cold exists, but the symptoms can be treated. Antibiotics have no effect against viral infections and thus have no effect against the viruses that cause the common cold. Due to their side effects they cause overall harm; however, they are still frequently prescribed. It is the most frequent infectious disease in humans with the average adult contracting two to three colds a year and the average child contracting between six and twelve. These infections have been with humanity since antiquity.
Allergies are a number of conditions caused by hypersensitivity of the immune system to typically harmless substances in the environment. These diseases include hay fever, food allergies, atopic dermatitis, allergic asthma, and anaphylaxis. Symptoms may include red eyes, an itchy rash, sneezing, a runny nose, shortness of breath, or swelling. Food intolerances and food poisoning are separate conditions.
Early exposure to potential allergens may be protective. Treatments for allergies include the avoidance of known allergens and the use of medications such as steroids and antihistamines. Histamine is concentrated in mast cells, cells whose function is essentially to release histamine and immunoglobins when tissue damage occurs. They are especially numerous in parts of the body that are injured often, such as the fingers and toes, or which enjoy frequent contact with the environment, such as the mucosa of the lips, nose, etc.
Types of Cold and Allergy Medications
Cold medicines are medications used by people with the common cold, cough, or related conditions. While a wide variety of drugs are marketed as cough suppressants, research shows there is often little or no measurable benefit in reducing cough symptoms. While they have been used by 10% of American children in any given week, they are not recommended in Canada or the United States in children six years or younger because of lack of evidence showing effect and concerns of harm. One version with codeine, guaifenesin, and pseudoephedrine was the 213th most commonly prescribed medication in 2017, in the United States, with more than two million prescriptions.
There are a number of different cough and cold medications, which may be used for various coughing symptoms. The commercially available products may include various combinations of any one or more of the following types of substances listed in the table below.
| Medication | Function | Examples |
|---|---|---|
| Mucokinetics, or mucolytics | a class of drugs which aid in the clearance of mucus from the airways, lungs, bronchi, and trachea | carbocisteine, ambroxol, and bromhexine. |
| Expectorants | substances claimed to make coughing easier while enhancing the production of mucus and phlegm. | acetylcysteine and guaifenesin. |
| Antitussives, or cough suppressants substances which suppress the coughing itself | substances which suppress the coughing itself | codeine, pholcodine, dextromethorphan, noscapine, and butamirate. |
| Antihistamines | for allergic rhinitis may produce mild sedation and reduce other associated symptoms, like a runny nose and watery eyes | diphenhydramine, chlorpheniramine, brompheniramine, loratadine, and cetirizine. |
| Decongestants | relieve nasal congestion and sinus infection | ephedrine, phenylephrine, pseudoephedrine, and oxymetazoline. |
| Fever or pain medication (antipyretic or analgesic) | fever reducer or pain reliever | paracetamol (called "acetaminophen " in the US) and NSAIDs such as aspirin, ibuprofen or naproxen |
| Syrups | various substances supposed to soften the coughing | honey or supplement syrup |
Effectiveness
The efficacy of cough medication is questionable, particularly in children. A 2014 Cochrane review concluded that "There is no good evidence for or against the effectiveness of OTC medicines in acute cough". Some cough medicines may be no more effective than placebos for acute coughs in adults, including coughs related to upper respiratory tract infections. The American College of Chest Physicians emphasizes that cough medicines are not designed to treat whooping cough, a cough that is caused by bacteria and can last for months. No over-the-counter cough medicines have been found to be effective in cases of pneumonia. They are not recommended in those who have COPD, chronic bronchitis, or the common cold. There is not enough evidence to make recommendations for those who have a cough and cancer.
Medications
- Dextromethorphan (DXM) may be modestly effective in decreasing cough in adults with viral upper respiratory infections. However, in children it has not been found to be effective.
- Codeine was once viewed as the "gold standard" in cough suppressants, but this position is now questioned. Some recent placebo-controlled trials have found that it may be no better than a placebo for some causes including acute cough in children. It is thus not recommended for children. Additionally, there is no evidence that hydrocodone is useful in children. Similarly, a 2012 Dutch guideline does not recommend its use to treat acute cough.
- A number of other commercially available cough treatments have not been shown to be effective in viral upper respiratory infections. These include for adults: antihistamines, antihistamine-decongestant combinations, benzonatate, anti asthmatic-expectorant-mucolytic combinations, expectorant-bronchodilator combinations, leukotriene inhibitors, ambroxol, and guaifenesin, sometimes with analgesics, antipyretics, anti inflammatories, and anticholinergics - and for children: antihistamines, decongestants for clearing the nose, or combinations of these and leukotriene inhibitors for allergy and asthma. However, antihistamines cannot be used as an empirical therapy in case of chronic, or non specific cough especially in very young children. Long term diphenhydramine use is associated with negative outcomes in older people.
Antihistamines are drugs which treat hay fever and other allergies. Typically, people take antihistamines as an inexpensive, not patented (generic), drug that can be bought without a prescription and relieves from nasal congestion, sneezing, or hives caused by pollen, dust mites, or animal allergy with few side effects. Antihistamines are usually for short-term treatment. Chronic allergies increase the risk of health problems which antihistamines might not treat, including asthma, sinusitis, and lower respiratory tract infection. Consultation of a medical professional is recommended for those who intend to take antihistamines for longer-term use.
Although people typically use the word “antihistamine” to describe drugs for treating allergies, doctors and scientists use the term to describe a class of drug that opposes the activity of histamine receptors in the body. In this sense of the word, antihistamines are subclassified according to the histamine receptor that they act upon. The two largest classes of antihistamines are H1-antihistamines and H2-antihistamines.
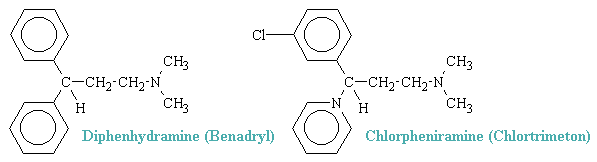
H1-antihistamines work by binding to histamine H1 receptors in mast cells, smooth muscle, and endothelium in the body as well as in the tuberomammillary nucleus in the brain. Antihistamines that target the histamine H1-receptor are used to treat allergic reactions in the nose (e.g., itching, runny nose, and sneezing). In addition, they may be used to treat insomnia, motion sickness, or vertigo caused by problems with the inner ear. H2-antihistamines bind to histamine H2 receptors in the upper gastrointestinal tract, primarily in the stomach. Antihistamines that target the histamine H2-receptor are used to treat gastric acid conditions (e.g., peptic ulcers and acid reflux). Two common examples of antihistamines are shown below.
Honey may be a minimally effective cough treatment. A Cochrane review found the evidence to recommend for or against its use in children to be weak. In light of this they found it was better than no treatment, placebo, and diphenhydramine but not better than dextromethorphan for relieving cough symptoms. Honey's use as a cough treatment has been linked on several occasions to infantile botulism and accordingly should not be used in children less than one year old.
Many alternative treatments are used to treat the common cold. A 2007 review states that, "alternative therapies (i.e., Echinacea, vitamin C, and zinc) are not recommended for treating common cold symptoms; however, ... Vitamin C prophylaxis may modestly reduce the duration and severity of the common cold in the general population and may reduce the incidence of the illness in persons exposed to physical and environmental stresses." A 2014 review also found insufficient evidence for Echinacea.
A 2009 review found that the evidence supporting the effectiveness of zinc is mixed with respect to cough, and a 2011 Cochrane review concluded that zinc "administered within 24 hours of onset of symptoms reduces the duration and severity of the common cold in healthy people". A 2003 review concluded: "Clinical trial data support the value of zinc in reducing the duration and severity of symptoms of the common cold when administered within 24 hours of the onset of common cold symptoms." Zinc gel in the nose may lead to long-term or permanent loss of smell. The FDA therefore discourages its use.
Adverse effects
A number of accidental overdoses and well-documented adverse effects suggested caution in children. The FDA in 2015 warned that the use of codeine-containing cough medication in children may cause breathing problems. Cold syrup overdose has been linked to visual and auditory hallucinations, rapid involuntary jaw, tongue and eye movements in children.
Summary
- The common cold (also known as nasopharyngitis, rhinopharyngitis, acute coryza, or a cold) is a viral infectious disease of the upper respiratory tract which affects primarily the nose. The symptoms of the common cold are believed to be primarily related to the immune response to the virus.
- An allergy is an immune response (with the release of histamines), or reaction, to substances (allergens) that are usually not harmful.
- A number of different cough and cold medications can be used to alleviate various symptoms but not diminish the intensity of the response.
Contributors
- Libretext: Microbiology (Boundless)
- Wikipedia

