18.3: Drugs and Infectious Diseases
- Page ID
- 152254
\( \newcommand{\vecs}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vecd}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash {#1}}} \)
\( \newcommand{\id}{\mathrm{id}}\) \( \newcommand{\Span}{\mathrm{span}}\)
( \newcommand{\kernel}{\mathrm{null}\,}\) \( \newcommand{\range}{\mathrm{range}\,}\)
\( \newcommand{\RealPart}{\mathrm{Re}}\) \( \newcommand{\ImaginaryPart}{\mathrm{Im}}\)
\( \newcommand{\Argument}{\mathrm{Arg}}\) \( \newcommand{\norm}[1]{\| #1 \|}\)
\( \newcommand{\inner}[2]{\langle #1, #2 \rangle}\)
\( \newcommand{\Span}{\mathrm{span}}\)
\( \newcommand{\id}{\mathrm{id}}\)
\( \newcommand{\Span}{\mathrm{span}}\)
\( \newcommand{\kernel}{\mathrm{null}\,}\)
\( \newcommand{\range}{\mathrm{range}\,}\)
\( \newcommand{\RealPart}{\mathrm{Re}}\)
\( \newcommand{\ImaginaryPart}{\mathrm{Im}}\)
\( \newcommand{\Argument}{\mathrm{Arg}}\)
\( \newcommand{\norm}[1]{\| #1 \|}\)
\( \newcommand{\inner}[2]{\langle #1, #2 \rangle}\)
\( \newcommand{\Span}{\mathrm{span}}\) \( \newcommand{\AA}{\unicode[.8,0]{x212B}}\)
\( \newcommand{\vectorA}[1]{\vec{#1}} % arrow\)
\( \newcommand{\vectorAt}[1]{\vec{\text{#1}}} % arrow\)
\( \newcommand{\vectorB}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vectorC}[1]{\textbf{#1}} \)
\( \newcommand{\vectorD}[1]{\overrightarrow{#1}} \)
\( \newcommand{\vectorDt}[1]{\overrightarrow{\text{#1}}} \)
\( \newcommand{\vectE}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash{\mathbf {#1}}}} \)
\( \newcommand{\vecs}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vecd}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash {#1}}} \)
\(\newcommand{\avec}{\mathbf a}\) \(\newcommand{\bvec}{\mathbf b}\) \(\newcommand{\cvec}{\mathbf c}\) \(\newcommand{\dvec}{\mathbf d}\) \(\newcommand{\dtil}{\widetilde{\mathbf d}}\) \(\newcommand{\evec}{\mathbf e}\) \(\newcommand{\fvec}{\mathbf f}\) \(\newcommand{\nvec}{\mathbf n}\) \(\newcommand{\pvec}{\mathbf p}\) \(\newcommand{\qvec}{\mathbf q}\) \(\newcommand{\svec}{\mathbf s}\) \(\newcommand{\tvec}{\mathbf t}\) \(\newcommand{\uvec}{\mathbf u}\) \(\newcommand{\vvec}{\mathbf v}\) \(\newcommand{\wvec}{\mathbf w}\) \(\newcommand{\xvec}{\mathbf x}\) \(\newcommand{\yvec}{\mathbf y}\) \(\newcommand{\zvec}{\mathbf z}\) \(\newcommand{\rvec}{\mathbf r}\) \(\newcommand{\mvec}{\mathbf m}\) \(\newcommand{\zerovec}{\mathbf 0}\) \(\newcommand{\onevec}{\mathbf 1}\) \(\newcommand{\real}{\mathbb R}\) \(\newcommand{\twovec}[2]{\left[\begin{array}{r}#1 \\ #2 \end{array}\right]}\) \(\newcommand{\ctwovec}[2]{\left[\begin{array}{c}#1 \\ #2 \end{array}\right]}\) \(\newcommand{\threevec}[3]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \end{array}\right]}\) \(\newcommand{\cthreevec}[3]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \end{array}\right]}\) \(\newcommand{\fourvec}[4]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \\ #4 \end{array}\right]}\) \(\newcommand{\cfourvec}[4]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \\ #4 \end{array}\right]}\) \(\newcommand{\fivevec}[5]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \\ #4 \\ #5 \\ \end{array}\right]}\) \(\newcommand{\cfivevec}[5]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \\ #4 \\ #5 \\ \end{array}\right]}\) \(\newcommand{\mattwo}[4]{\left[\begin{array}{rr}#1 \amp #2 \\ #3 \amp #4 \\ \end{array}\right]}\) \(\newcommand{\laspan}[1]{\text{Span}\{#1\}}\) \(\newcommand{\bcal}{\cal B}\) \(\newcommand{\ccal}{\cal C}\) \(\newcommand{\scal}{\cal S}\) \(\newcommand{\wcal}{\cal W}\) \(\newcommand{\ecal}{\cal E}\) \(\newcommand{\coords}[2]{\left\{#1\right\}_{#2}}\) \(\newcommand{\gray}[1]{\color{gray}{#1}}\) \(\newcommand{\lgray}[1]{\color{lightgray}{#1}}\) \(\newcommand{\rank}{\operatorname{rank}}\) \(\newcommand{\row}{\text{Row}}\) \(\newcommand{\col}{\text{Col}}\) \(\renewcommand{\row}{\text{Row}}\) \(\newcommand{\nul}{\text{Nul}}\) \(\newcommand{\var}{\text{Var}}\) \(\newcommand{\corr}{\text{corr}}\) \(\newcommand{\len}[1]{\left|#1\right|}\) \(\newcommand{\bbar}{\overline{\bvec}}\) \(\newcommand{\bhat}{\widehat{\bvec}}\) \(\newcommand{\bperp}{\bvec^\perp}\) \(\newcommand{\xhat}{\widehat{\xvec}}\) \(\newcommand{\vhat}{\widehat{\vvec}}\) \(\newcommand{\uhat}{\widehat{\uvec}}\) \(\newcommand{\what}{\widehat{\wvec}}\) \(\newcommand{\Sighat}{\widehat{\Sigma}}\) \(\newcommand{\lt}{<}\) \(\newcommand{\gt}{>}\) \(\newcommand{\amp}{&}\) \(\definecolor{fillinmathshade}{gray}{0.9}\)- Differentiate between antibiotics and antiviral agents.
- Know the different antibiotics and antiviral agents and their mode of action.
The World Health Organization’s (WHO) International Classification of Diseases (ICD) is used in clinical fields to classify diseases and monitor morbidity (the number of cases of a disease) and mortality (the number of deaths due to a disease). In this section, we will introduce terminology used by the ICD (and in health-care professions in general) to describe and categorize various types of disease.
An infectious disease is any disease caused by the direct effect of a pathogen. A pathogen may be cellular (bacteria, parasites, and fungi) or acellular (viruses, viroids, and prions). Some infectious diseases are also communicable, meaning they are capable of being spread from person to person through either direct or indirect mechanisms. Some infectious communicable diseases are also considered contagious diseases, meaning they are easily spread from person to person. Not all contagious diseases are equally so; the degree to which a disease is contagious usually depends on how the pathogen is transmitted. For example, measles is a highly contagious viral disease that can be transmitted when an infected person coughs or sneezes and an uninfected person breathes in droplets containing the virus. Gonorrhea is not as contagious as measles because transmission of the pathogen (Neisseria gonorrhoeae) requires close intimate contact (usually sexual) between an infected person and an uninfected person.
Antibiotics
The modern era of the chemotherapy of infection started with the clinical use of sulfanilamide in 1936. The "golden age" of antimicrobial therapy began with the production of penicillin in 1941, when this compound was mass-produced and first made available for limited clinical trial. More than 30% of all hospitalized patients now receive one or more courses of therapy with antibiotics, and millions of potentially fatal infections have been cured. However, at the same time, these pharmaceutical agents have become among the most misused of those available to the practicing physician. One result of widespread use of antimicrobial agents has been the emergence of antibiotic-resistant pathogens, which in turn has created an ever-increasing need for new drugs. Many of these agents have also contributed significantly to the rising costs of medical care.
An antibiotic is any substance produced by a microorganism that is excreted to harm or kill another microorganism. Technically, antibiotics are microbial or fungal products. But these substances can be synthesized and mass produced in the laboratory to use against harmful microorganisms in the environment. Thus, the synthetic chemist has added greatly to our therapeutic armamentarium. Synthetic drugs such as isonaizid and theambutol represent important contributions for the treatment of tuberculosis. While many such antimicrobial agents are not properly termed antibiotics, since they are not produced by living organisms, little distinction should now be made between compounds of natural and synthetic origin.
Synthetic Antibiotics - Sulfonamides
Sulfonamide is the basis of several groups of drugs. The original antibacterial sulfonamides (sometimes called sulfa drugs or sulpha drugs) are synthetic antimicrobial agents that contain the sulfonamide group. Some sulfonamides are also devoid of antibacterial activity, e.g., the anticonvulsant sultiame. The sulfonylureas and thiazide diuretics are newer drug groups based on the antibacterial sulfonamides.
Sulfa allergies are common, and medications containing sulfonamides are prescribed carefully. It is important to make a distinction between sulfa drugs and other sulfur-containing drugs and additives, such as sulfates and sulfites, which are chemically unrelated to the sulfonamide group and do not cause the same hypersensitivity reactions seen in the sulfonamides.
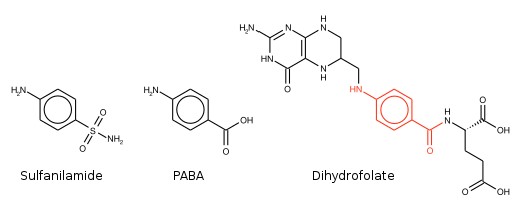
Sulfonamides are structural analogs and competitive antagonists of para-aminobenzoic acid (PABA), and thus prevent normal bacterial utilization of PABA for the synthesis of the vitamin folic acid (Figure \(\PageIndex{1}\)). More specifically, sulfonamides are competitive inhibitors of the bacterial enzyme sulfihydropteroate synthase, which is responsible for the conversion of PABA into dihydrofolic acid, the immediate precursor of folic acid. Sensitive microorganisms are those that must synthesis their own folic acid; bacteria that can utilize preformed folic acid are not affected.
Cell Wall Synthesis Inhibitors - Penicillin and Cepalosphorins
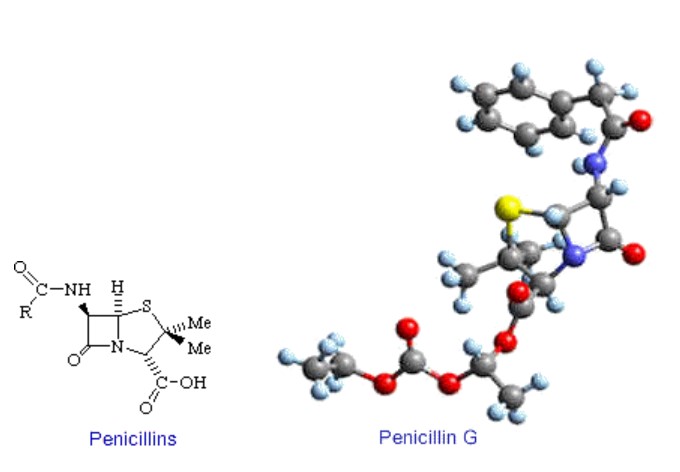
The penicillins were the first antibiotics discovered as natural products from the mold Penicillium and was effective against Gram-positive bacteria. All penicillin derivatives produce their bacteriocidal effects by inhibition of bacterial cell wall synthesis. Specifically, the cross linking of peptides on the mucosaccharide chains is prevented. If cell walls are improperly made cell walls allow water to flow into the cell causing it to burst. A number of natural penicillins have been discovered, but only two purified compounds are in clinical use: penicillin G (intravenous use) and penicillin V (given by mouth). Several semisynthetic penicillins are effective against a broader spectrum of bacteria: these include the antistaphylococcal penicillins, aminopenicillins and the antipseudomonal penicillins.
Like penicillin, cephalosporins are valuable because of their low toxicity and their broad spectrum of action against various diseases. In this way, cephalosporin is very similar to penicillin. Cephalosporins are one of the most widely used antibiotics, and economically speaking, has about 29% of the antibiotic market. The cephalosporins are possibly the single most important group of antibiotics today and are equal in importance to penicillin. The structure and mode of action of the cephalosporins are similar to that of penicillin. They affect bacterial growth by inhibiting cell wall synthesis, in Gram-positive and -negative bacteria.
Figure \(\PageIndex{3}\) Cephalosporins.
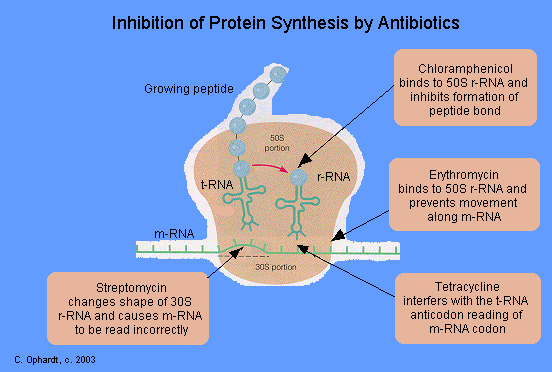
Protein Synthesis Inhibitors - Erythromycin, Tetracycline, Streptomycin, and Chloramphenicol
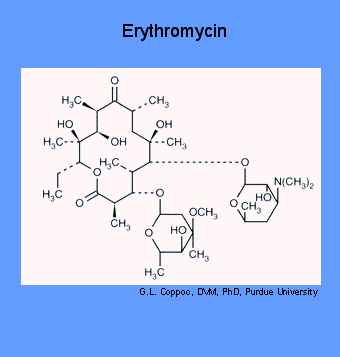
Erythromycin is an orally effective antibiotic discovered in 1952 in the metabolic products of a strain of Streptocyces erythreus, originally obtained from a soil sample collected in the Philippine Archipelago. Erythromycin may be either bacteriostatic or bactericidal, depending on the microorganism and the concentration of the drug.
Erythromycin is an antibiotic used for the treatment of a number of bacterial infections. This includes respiratory tract infections, skin infections, chlamydia infections, pelvic inflammatory disease, and syphilis. It may also be used during pregnancy to prevent Group B streptococcal infection in the newborn, as well as to improve delayed stomach emptying. It can be given intravenously and by mouth. An eye ointment is routinely recommended after delivery to prevent eye infections in the newborn.
Erythromycin and other macrolide antibiotics inhibit protein synthesis by binding to 50 S ribosomal subunits of sensitive microorganisms. (Humans do not have 50 S ribosomal subunits, but have ribosomes composed of 40 S and 60 S subunits). Certain resistant microorganisms with mutational changes in components of this subunit of the ribosome fail to bind the drug.
Tetracyclines have the broadest spectrum of antimicrobial activity. These may include: Aureomycin, Terramycin, and Panmycin. Four fused 6-membered rings, as shown in the figure below, form the basic structure from which the various tetracyclines are made. The various derivatives are different at one or more of four sites on the rigid, planar ring structure. The classical tetracyclines were derived from Streptomyces spp., but the newer derivatives are semisynthetic as is generally true for newer members of other drug groups.
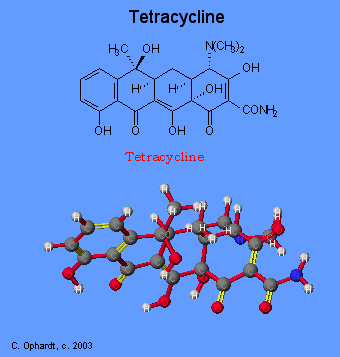
Tetracyclines inhibit bacterial protein synthesis by blocking the attachment of the transfer RNA-amino acid to the ribosome. More precisely they are inhibitors of the codon-anticodon interaction. Tetracyclines can also inhibit protein synthesis in the host, but are less likely to reach the concentration required because eukaryotic cells do not have a tetracycline uptake mechanism.
Streptomycin
Streptomycin is effective against gram-negative bacteria, although it is also used in the treatment of tuberculosis. Streptomycin binds to the 30S ribosome and changes its shape so that it and inhibits protein synthesis by causing a misreading of messenger RNA information.
Chloramphenicol
Chloromycetin is also a broad spectrum antibiotic that possesses activity similar to the tetracylines. At present, it is the only antibiotic prepared synthetically. It is reserved for treatment of serious infections because it is potentially highly toxic to bone marrow cells. It inhibits protein synthesis by attaching to the ribosome and interferes with the formation of peptide bonds between amino acids. It behaves as an antimetabolite for the essential amino acid phenylalanine at ribosomal binding sites.
| Antibiotic | Producer organism | Activity | Site or mode of action |
|---|---|---|---|
| Penicillin | Penicillium chrysogenum | Gram-positive bacteria | Wall synthesis |
| Cephalosporin | Cephalosporium acremonium | Broad spectrum | Wall synthesis |
| Griseofulvin | Penicillium griseofulvum | Dermatophytic fungi | Microtubules |
| Bacitracin | Bacillus subtilis | Gram-positive bacteria | Wall synthesis |
| Polymyxin B | Bacillus polymyxa | Gram-negative bacteria | Cell membrane |
| Amphotericin B | Streptomyces nodosus | Fungi | Cell membrane |
| Erythromycin | Streptomyces erythreus | Gram-positive bacteria | Protein synthesis |
| Neomycin | Streptomyces fradiae | Broad spectrum | Protein synthesis |
| Streptomycin | Streptomyces griseus | Gram-negative bacteria | Protein synthesis |
| Tetracycline | Streptomyces rimosus | Broad spectrum | Protein synthesis |
| Vancomycin | Streptomyces orientalis | Gram-positive bacteria | Protein synthesis |
| Gentamicin | Micromonospora purpurea | Broad spectrum | Protein synthesis |
| Rifamycin | Streptomyces mediterranei | Tuberculosis | Protein synthesis |
Alexander Fleming loved to play, both in the laboratory and out. He always loved snooker and golf and had many whimsical variants on the rules. In the lab he made "germ paintings," in which he would draw with his culture loop using spores of highly pigmented bacteria, which were invisible when he made the painting, but when cultured developed into brightly colored scenes. He followed what Max Delbruck would later call the "principle of limited sloppiness." Fleming abhorred a tidy, meticulous lab; he left culture dishes lying around for weeks and would often discover interesting things in them. Though the story has been told in many sometimes conflicting ways, something like this resulted in the discovery of penicillin. He seems to have left a culture dish lying on the lab bench and then gone away on vacation. When he returned a few spores of an unusual mold had germinated on the plate. When he cultured the bacteria on the plate he found that they grew up to within a few centimeters of the mold, but there were killed. A crude extract of the mold was then shown to have antibacterial properties. Fleming made this discovery in 1928 and by 1929 had named it penicillin (he was told by a colleague that the mold was a type of Penicillium and "penicillozyme" must have seemed cumbersome).
Fleming continued to use penicillin in his lab but not with any great enthusiasm and certainly not to the exclusion of many other projects. He never developed it into a clinically useful compound, though in 1929 he suggested that it might have important clinical applications. Because he was a bacteriologist and not a chemist, Fleming did not attempt to purify penicillin. He seems to have run into a dead end with penicillin and so during the 1930s, though he kept it in his lab, he did not do much with it. In the late 1930s Australian Howard Florey came to London to work with Charles Sherrington. He worked on lysozyme for a while and then became interested in penicillin. It was Florey, with Chain and other of his group that developed penicillin into a clinical antibiotic. They did this during 1940-41. Fleming, Florey, and Chain shared the 1945 Nobel Prize in Physiology for Medicine.
Fleming became world-famous for penicillin, and was rightly acknowledged as the father of modern antibiotics, but Florey was just as rightly miffed at being denied much of the credit for creating the powerful medical tool we now know. Evidence does not suggest that Fleming deliberately denied Florey his due credit, but Fleming's peculiar, dry sense of humor seems to have caused him not to deny even the wildest attributions to him.
Viruses and Antiviral Drugs
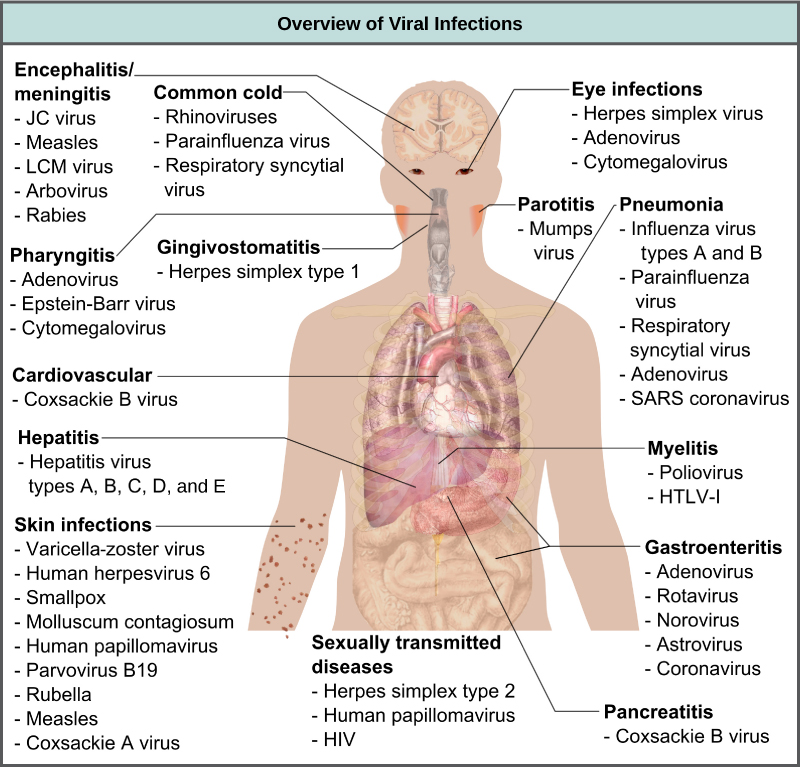
Viruses cause a variety of diseases in animals, including humans, ranging from the common cold to potentially fatal illnesses like meningitis (FIgure \(\PageIndex{1}\)). These diseases can be treated by antiviral drugs or by vaccines, but some viruses, such as HIV, are capable of both avoiding the immune response and mutating to become resistant to antiviral drugs.
Antiviral drugs are a class of medication used for treating viral infections. Most antivirals target specific viruses, while a broad-spectrum antiviral is effective against a wide range of viruses. Unlike most antibiotics, antiviral drugs do not destroy their target pathogen; instead they inhibit its development.
Antiviral drugs are one class of antimicrobials, a larger group which also includes antibiotic (also termed antibacterial), antifungal and antiparasitic drugs, or antiviral drugs based on monoclonal antibodies. Most antivirals are considered relatively to the host, and therefore can be used to treat infections. They should be distinguished from viricides, which are not medication but deactivate or destroy virus particles, either inside or outside the body. Natural viricides are produced by some plants such as eucalyptus and Australian tea trees.
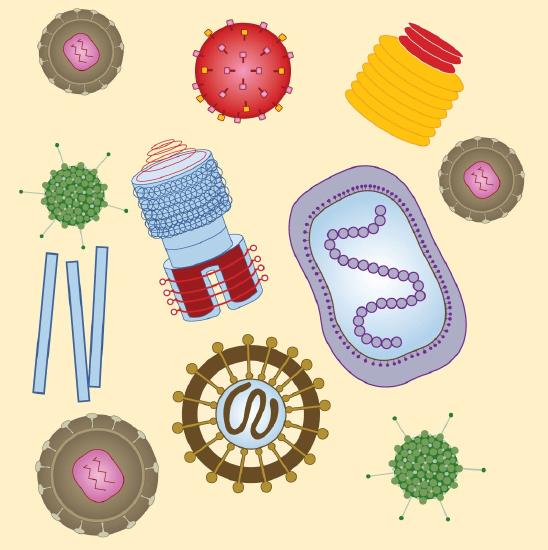
DNA Viruses and RNA Viruses
Viruses are visible only under an electron microscope. They come in a variety of shapes, ranging from spherical to rod shaped. The fact that they contain either deoxyribonucleic acid (DNA) or ribonucleic acid (RNA)—but never both—allows them to be divided into two major classes: DNA viruses and RNA viruses (Figure \(\PageIndex{1}\)).
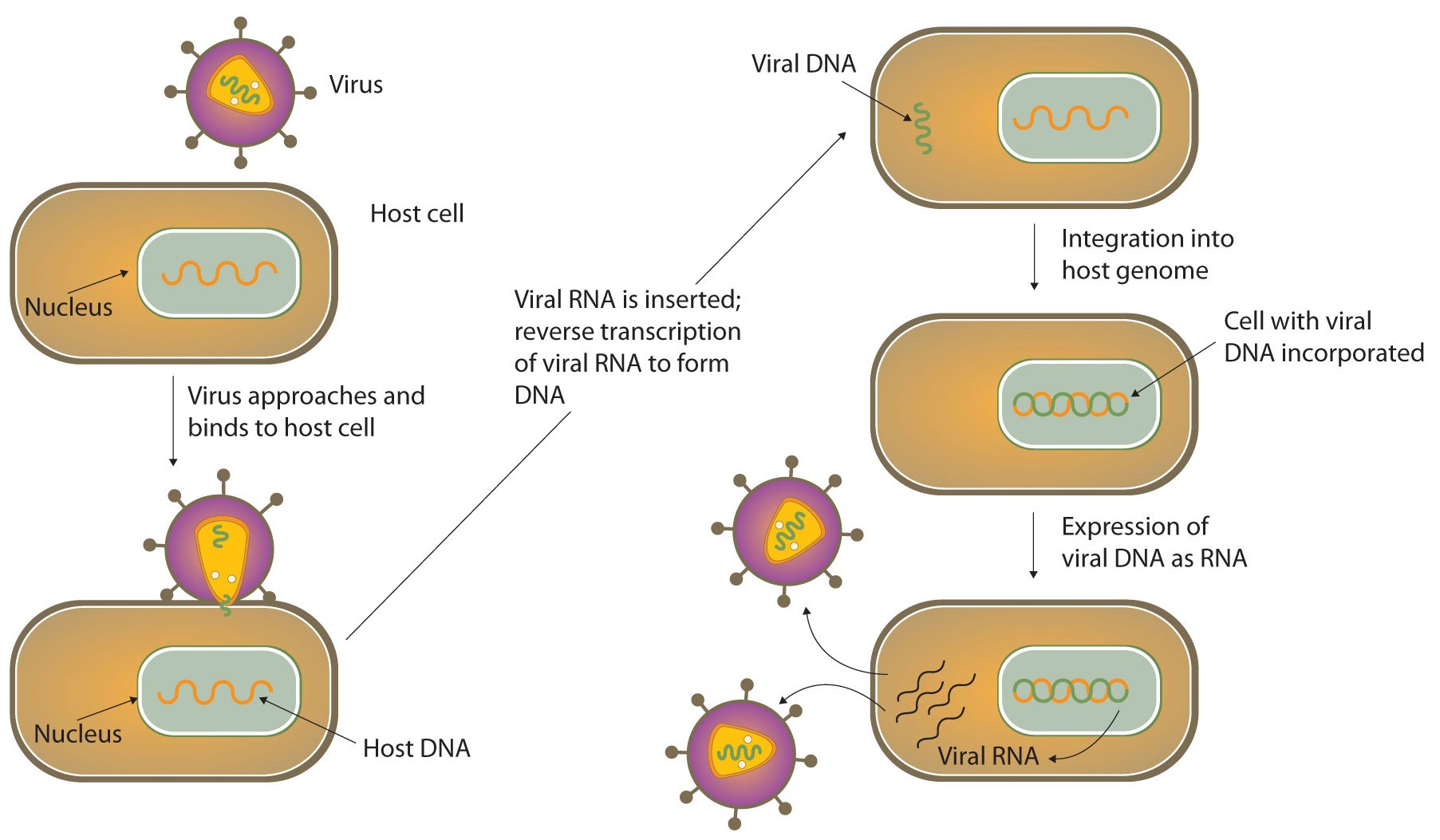
Most RNA viruses use their nucleic acids in much the same way as the DNA viruses, penetrating a host cell and inducing it to replicate the viral RNA and synthesize viral proteins. The new RNA strands and viral proteins are then assembled into new viruses. Some RNA viruses, however, called retroviruses (Figure \(\PageIndex{2}\)), synthesize DNA in the host cell, in a process that is the reverse of the DNA-to-RNA transcription that normally occurs in cells. The synthesis of DNA from an RNA template is catalyzed by the enzyme reverse transcriptase.
Anti-viral Drugs
Antiviral drugs often have limited success in curing viral disease, but in many cases, they have been used to control and reduce symptoms for a wide variety of viral diseases. For most viruses, these drugs can inhibit the virus by blocking the actions of one or more of its proteins. It is important that the targeted proteins be encoded by viral genes and that these molecules are not present in a healthy host cell. In this way, viral growth is inhibited without damaging the host. There are large numbers of antiviral drugs available to treat infections, some specific for a particular virus and others that can affect multiple viruses.
Antivirals have been developed to treat genital herpes (herpes simplex II) and influenza. For genital herpes, drugs such as acyclovir can reduce the number and duration of episodes of active viral disease, during which patients develop viral lesions in their skin cells. As the virus remains latent in nervous tissue of the body for life, this drug is not curative but can make the symptoms of the disease more manageable. For influenza, drugs like Tamiflu (oseltamivir) (Figure \(\PageIndex{3}\)) can reduce the duration of “flu” symptoms by 1 or 2 days, but the drug does not prevent symptoms entirely. Tamiflu works by inhibiting an enzyme (viral neuraminidase) that allows new virions to leave their infected cells. Thus, Tamiflu inhibits the spread of virus from infected to uninfected cells. Other antiviral drugs, such as Ribavirin, have been used to treat a variety of viral infections, although its mechanism of action against certain viruses remains unclear.
By far, the most successful use of antivirals has been in the treatment of the retrovirus HIV, which causes a disease that, if untreated, is usually fatal within 10–12 years after infection. Anti-HIV drugs have been able to control viral replication to the point that individuals receiving these drugs survive for a significantly longer time than the untreated.
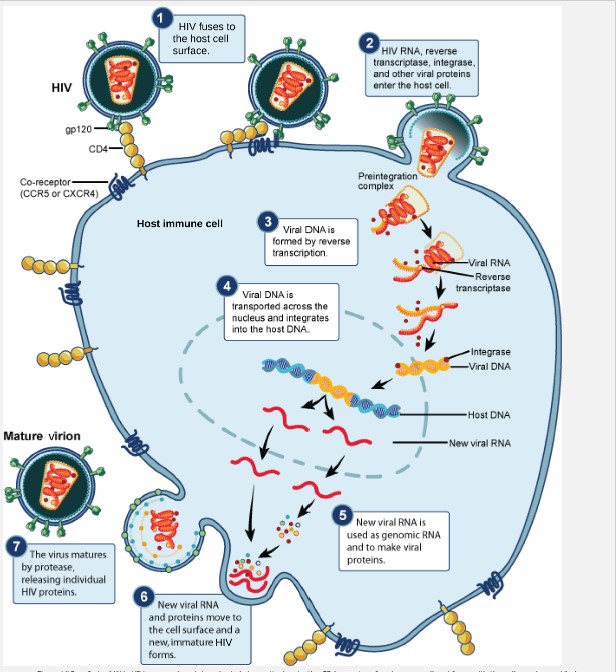
Anti-HIV drugs inhibit viral replication at many different phases of the HIV replicative cycle (Figure \(\PageIndex{4}\)). Drugs have been developed that inhibit the fusion of the HIV viral envelope with the plasma membrane of the host cell (fusion inhibitors), the conversion of its RNA genome into double-stranded DNA (reverse transcriptase inhibitors), the integration of the viral DNA into the host genome (integrase inhibitors), and the processing of viral proteins (protease inhibitors).
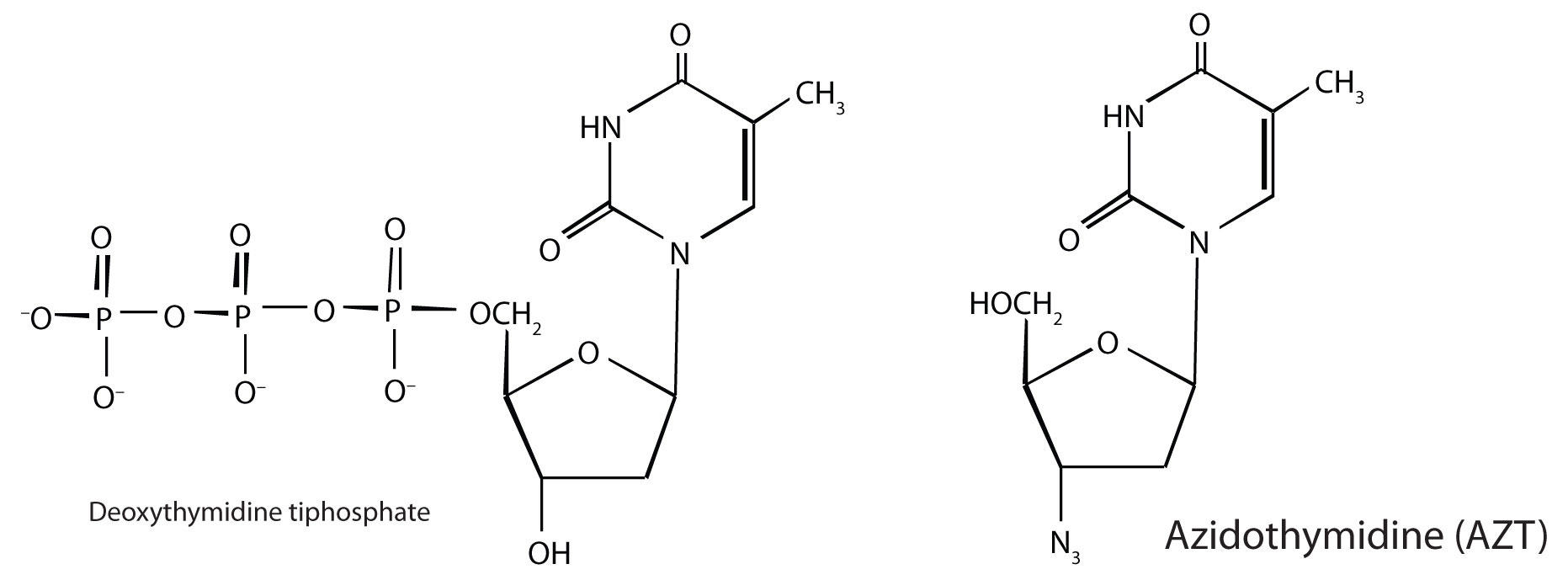
In 1987, azidothymidine (AZT, also known as zidovudine or the brand name Retrovir) became the first drug approved for the treatment of AIDS. It works by binding to reverse transcriptase in place of deoxythymidine triphosphate, after which, because AZT does not have a 3′OH group, further replication is blocked. In the past 10 years, several other drugs have been approved that also act by inhibiting the viral reverse transcriptase.
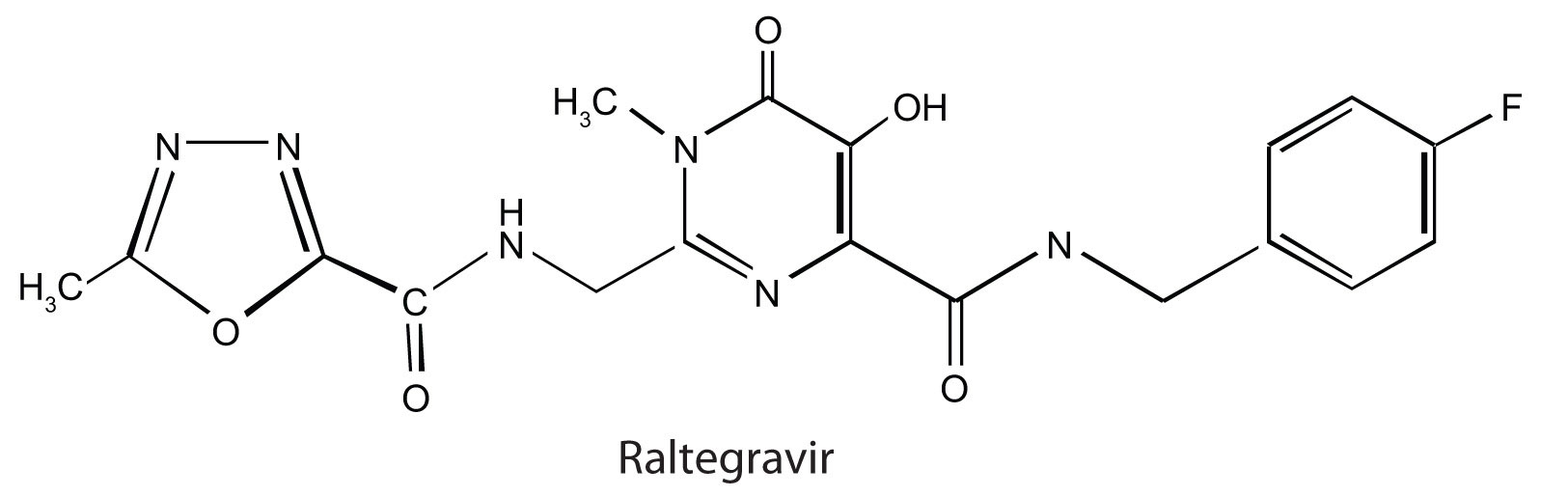
Raltegravir (Isentress) is a newer anti-AIDS drug that was approved by the FDA in October 2007. This drug inhibits the integrase enzyme that is needed to integrate the HIV DNA into cellular DNA, an essential step in the production of more HIV particles.
A major problem in treating HIV infections is that the virus can become resistant to any of these drugs. One way to combat the problem has been to administer a “cocktail” of drugs, typically a combination of two reverse transcriptase inhibitors along with a protease inhibitor. These treatments can significantly reduce the amount of HIV in an infected person.
The management of HIV/AIDS normally includes the use of multiple antiretroviral drugs in an attempt to control HIV infection. There are several classes of antiretroviral agents that act on different stages of the HIV life-cycle. The use of multiple drugs that act on different viral targets is known as highly active antiretroviral therapy (HAART). HAART decreases the patient's total burden of HIV, maintains function of the immune system, and prevents opportunistic infections that often lead to death. HAART also prevents the transmission of HIV between serodiscordant same sex and opposite sex partners so long as the HIV-positive partner maintains an undetectable viral load.
A more detailed list of antivirals other than HIV is given in Table \(\PageIndex{1}\).
| Antiviral | Brand Name | Use |
|---|---|---|
| amantadine | Symmetrel | used prophylactically against influenza A ) in high-risk individuals. It prevents influenza A viruses from the uncoating step necessary for viral replication. |
| rimantidine | Flumadine | used for treatment and prophylaxis of influenza A. It prevents influenza A viruses from the uncoating step necessary for viral replication. |
| zanamivir: | Relenza | used to limit the duration of influenza A and B infections. It is an inhibitor of the influenza virus surface enzyme called neuraminidase that is needed for release of newly formed influenza viruses from the infected cell. |
| oseltamivir | Tamiflu | used limit the duration of influenza infections. It is an inhibitor of the influenza virus surface enzyme called neuraminidase that is needed for release of newly formed influenza viruses from the infected cell. |
| acyclovir | Zovirax | used against herpes simplex viruses (HSV) to treat genital herpes, mucocutaneous herpes in the immunosuppressed, HSV encephalitis, neonatal herpes, and to reduce the rate of recurrences of genital herpes. It is also used against varicella zoster viruses (VZV) ) to treat shingles. It chemically resembles a normal DNA nucleoside. Once inserted into the growing DNA chain it inhibits further viral DNA replication. |
| trifluridine | Viroptic | used to treat eye infection (keratitis and conjunctivitis) caused by HSV. It chemically resembles a normal DNA nucleoside. Once inserted into the growing DNA chain it inhibits further viral DNA replication. |
| famciclovir | Famvir | used to treat HSV and VZV infections. It chemically resembles a normal DNA nucleoside. Once inserted into the growing DNA chain it inhibits further viral DNA replication. |
| valacyclovir | Valtrex | used to treat HSV and VZV infections. It chemically resembles a normal DNA nucleoside. Once inserted into the growing DNA chain it inhibits further viral DNA replication. |
| penciclovir | Denavir | used in treating HSV infections. It chemically resembles a normal DNA nucleoside. Once inserted into the growing DNA chain it inhibits further viral DNA replication. |
| gancyclovir | Cytovene; Vitrasert | used in treating severe cytomegalovirus (CMV) infections such as retinitis. It chemically resembles a normal DNA nucleoside. Once inserted into the growing DNA chain it inhibits further viral DNA replication. |
| valganciclovir | Valcyte | used in treating severe CMV infections such as retinitis). It chemically resembles a normal DNA nucleoside. Once inserted into the growing DNA chain it inhibits further viral DNA replication. |
| foscarnet | Foscavir | used in treating severe CMV infections such as retinitis. It chemically resembles a normal DNA nucleoside. Once inserted into the growing DNA chain it inhibits further viral DNA replication. |
| cidofovir | Vistide | used in treating CMV retinitis. It chemically resembles a normal DNA nucleoside. Once inserted into the growing DNA chain it inhibits further viral DNA replication. |
| fomivirsen | Vitravene | used in treating CMV retinitis. Fomivirsen inhibits cytomegalovirus (CMV) replication through an antisense RNA (microRNA or miRNA mechanism. The nucleotide sequence of fomivirsen is complementary to a sequence in mRNA transcripts (Figure \(\PageIndex{1}\)) that encodes several proteins responsible for regulation of viral gene expression that are essential for production of infectious CMV. Binding of fomivirsen to the target mRNA results in inhibition of protein synthesis, subsequently inhibiting virus replication. |
| ribavirin | Copegus; Rebetol; Virazole | used in treating severe acute respiratory syndrome (SARS). In combination with other drugs it is used to treat hepatitis C virus (HCV). It chemically resembles a normal RNA nucleoside. Once inserted into the growing RNA chain it inhibits further viral RNA replication. |
| telaprevir | Incivek | for the treatment of chronic hepatitis C (hepatitis C virus or HCV genotype 1). It is a protease inhibitor that binds to the active site of an HCV-encoded protease and prevent it from cleaving the long polyprotein from polycistronic HCV genes into proteins essential to the structure and function of HCV. |
boceprevir |
Victrelis | for the treatment of chronic hepatitis C (hepatitis C virus or HCV genotype 1) infection. It is used in combination with peginterferon alfa and ribavirin. Boceprevir is a protease inhibitor that binds to the active site of an HCV-encoded protease and prevent it from cleaving the long polyprotein from polycistronic HCV genes into proteins essential to the structure and function of HCV. |
| simeprevir | Olysio | use for the treatment of chronic hepatitis C (hepatitis C virus or HCV genotype 1) infection. Used in combination with peginterferon alfa and ribavirin. Simeprevir is a protease inhibitor that binds to the active site of an HCV-encoded protease and prevent it from cleaving the long polyprotein from polycistronic HCV genes into proteins essential to the structure and function of HCV. |
| sofosbuvir | Sovaldi | Use for the treatment of chronic hepatitis C infection. Used in combination with ribavirin for hepatitis C virus or HCV genotypes 2 and 4; used in combination with peginterferon alfa and ribavirin for HCV genotypes 1 and 4. The second indication is the first approval of an interferon-free regimen for the treatment of chronic HCV infection. Sofosbuvir is a nucleotide polymerase inhibitor that binds to the active site of an HCV-encoded RNA polymerase preventing the synthesis of the viral RNA genome. |
| lamivudine | Epivir-HBV | used in treating chronic hepatitis B. It chemically resembles a normal DNA nucleoside. Once inserted into the growing DNA chain it inhibits further viral DNA replication. |
| adefovir dipivoxil | Hepsera | used in treating hepatitis B. |
A list of FDA-approved Antiretroviral drugs (last updated on April 12, 2018) used in the treatment of HIV infection can be found on the website: www.fda.gov/patients/hiv-treatment/antiretroviral-drugs-used-treatment-hiv-infection
Basic Research and Drug Development
The general idea behind modern antiviral drug design is to identify viral proteins, or parts of proteins, that can be disabled. These "targets" should generally be as unlike any proteins or parts of proteins in humans as possible, to reduce the likelihood of side effects. The targets should also be common across many strains of a virus, or even among different species of virus in the same family, so a single drug will have broad effectiveness. For example, a researcher might target a critical enzyme synthesized by the virus, but not by the patient, that is common across strains, and see what can be done to interfere with its operation.
Once targets are identified, candidate drugs can be selected, either from drugs already known to have appropriate effects or by actually designing the candidate at the molecular level with a computer-aided design program.
The target proteins can be manufactured in the lab for testing with candidate treatments by inserting the gene that synthesizes the target protein into bacteria or other kinds of cells. The cells are then cultured for mass production of the protein, which can then be exposed to various treatment candidates and evaluated with "rapid screening" technologies.
Prevention of Viral Diseases with Vaccination
While we do have limited numbers of effective antiviral drugs, such as those used to treat HIV and influenza, the primary method of controlling viral disease is by vaccination, which is intended to prevent outbreaks by building immunity to a virus or virus family (Figure \(\PageIndex{1}\)). Vaccines may be prepared using live viruses, killed viruses, or molecular subunits of the virus. The killed viral vaccines and subunit viruses are both incapable of causing disease.
Live viral vaccines are designed in the laboratory to cause few symptoms in recipients while giving them protective immunity against future infections. Polio was one disease that represented a milestone in the use of vaccines. Mass immunization campaigns in the 1950s (killed vaccine) and 1960s (live vaccine) significantly reduced the incidence of the disease, which caused muscle paralysis in children and generated a great amount of fear in the general population when regional epidemics occurred. The success of the polio vaccine paved the way for the routine dispensation of childhood vaccines against measles, mumps, rubella, chickenpox, and other diseases.
The danger of using live vaccines, which are usually more effective than killed vaccines, is the low but significant danger that these viruses will revert to their disease-causing form by back mutations. Live vaccines are usually made by attenuating (weakening) the “wild-type” (disease-causing) virus by growing it in the laboratory in tissues or at temperatures different from what the virus is accustomed to in the host. Adaptations to these new cells or temperatures induce mutations in the genomes of the virus, allowing it to grow better in the laboratory while inhibiting its ability to cause disease when reintroduced into conditions found in the host. These attenuated viruses thus still cause infection, but they do not grow very well, allowing the immune response to develop in time to prevent major disease. Back mutations occur when the vaccine undergoes mutations in the host such that it readapts to the host and can again cause disease, which can then be spread to other humans in an epidemic. This type of scenario happened as recently as 2007 in Nigeria where mutations in a polio vaccine led to an epidemic of polio in that country.
Some vaccines are in continuous development because certain viruses, such as influenza and HIV, have a high mutation rate compared to other viruses and normal host cells. With influenza, mutations in the surface molecules of the virus help the organism evade the protective immunity that may have been obtained in a previous influenza season, making it necessary for individuals to get vaccinated every year. Other viruses, such as those that cause the childhood diseases measles, mumps, and rubella, mutate so infrequently that the same vaccine is used year after year.

Summary
- An infectious disease is any disease caused by the direct effect of a pathogen (bacteria, parasites, fungi, viruses, viroids, and prions).
- Diseases can either be noninfectious (due to genetics and environment) or infectious (due to pathogens). Some infectious diseases are communicable (transmissible between individuals) or contagious (easily transmissible between individuals); others are noncommunicable, but may be contracted via contact with environmental reservoirs or animal.
- An antibiotic is any substance produced by a microorganism that is excreted to harm or kill another microorganism. Technically, antibiotics are microbial or fungal products.
- Most antibiotics inhibit bacterial growth by inhibiting cell wall synthesis or protein synthesis.
- Antiviral drugs are a class of medication used for treating viral infections. Most antivirals target specific viruses, while a broad-spectrum antiviral is effective against a wide range of viruses.
- The management of HIV/AIDS normally includes the use of multiple in an attempt to control .
- The primary method of controlling viral disease is by vaccination, which is intended to prevent outbreaks by building immunity to a virus or virus family
Contributors and Attributions
- Template:ContribOpenSTAXMicrobiology
- Template:ContribOpenSTAXGeneralBiology
Charles Ophardt (Professor Emeritus, Elmhurst College); Virtual Chembook
Dr. Gary Kaiser (COMMUNITY COLLEGE OF BALTIMORE COUNTY, CATONSVILLE CAMPUS)
- Wikipedia
- NIH MedlinePlus
- US FDA
- Libretext: The Basics of GOB Chemistry (Ball et al

