18.5: Hormones - The Regulators
- Page ID
- 152256
\( \newcommand{\vecs}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vecd}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash {#1}}} \)
\( \newcommand{\id}{\mathrm{id}}\) \( \newcommand{\Span}{\mathrm{span}}\)
( \newcommand{\kernel}{\mathrm{null}\,}\) \( \newcommand{\range}{\mathrm{range}\,}\)
\( \newcommand{\RealPart}{\mathrm{Re}}\) \( \newcommand{\ImaginaryPart}{\mathrm{Im}}\)
\( \newcommand{\Argument}{\mathrm{Arg}}\) \( \newcommand{\norm}[1]{\| #1 \|}\)
\( \newcommand{\inner}[2]{\langle #1, #2 \rangle}\)
\( \newcommand{\Span}{\mathrm{span}}\)
\( \newcommand{\id}{\mathrm{id}}\)
\( \newcommand{\Span}{\mathrm{span}}\)
\( \newcommand{\kernel}{\mathrm{null}\,}\)
\( \newcommand{\range}{\mathrm{range}\,}\)
\( \newcommand{\RealPart}{\mathrm{Re}}\)
\( \newcommand{\ImaginaryPart}{\mathrm{Im}}\)
\( \newcommand{\Argument}{\mathrm{Arg}}\)
\( \newcommand{\norm}[1]{\| #1 \|}\)
\( \newcommand{\inner}[2]{\langle #1, #2 \rangle}\)
\( \newcommand{\Span}{\mathrm{span}}\) \( \newcommand{\AA}{\unicode[.8,0]{x212B}}\)
\( \newcommand{\vectorA}[1]{\vec{#1}} % arrow\)
\( \newcommand{\vectorAt}[1]{\vec{\text{#1}}} % arrow\)
\( \newcommand{\vectorB}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vectorC}[1]{\textbf{#1}} \)
\( \newcommand{\vectorD}[1]{\overrightarrow{#1}} \)
\( \newcommand{\vectorDt}[1]{\overrightarrow{\text{#1}}} \)
\( \newcommand{\vectE}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash{\mathbf {#1}}}} \)
\( \newcommand{\vecs}[1]{\overset { \scriptstyle \rightharpoonup} {\mathbf{#1}} } \)
\( \newcommand{\vecd}[1]{\overset{-\!-\!\rightharpoonup}{\vphantom{a}\smash {#1}}} \)
\(\newcommand{\avec}{\mathbf a}\) \(\newcommand{\bvec}{\mathbf b}\) \(\newcommand{\cvec}{\mathbf c}\) \(\newcommand{\dvec}{\mathbf d}\) \(\newcommand{\dtil}{\widetilde{\mathbf d}}\) \(\newcommand{\evec}{\mathbf e}\) \(\newcommand{\fvec}{\mathbf f}\) \(\newcommand{\nvec}{\mathbf n}\) \(\newcommand{\pvec}{\mathbf p}\) \(\newcommand{\qvec}{\mathbf q}\) \(\newcommand{\svec}{\mathbf s}\) \(\newcommand{\tvec}{\mathbf t}\) \(\newcommand{\uvec}{\mathbf u}\) \(\newcommand{\vvec}{\mathbf v}\) \(\newcommand{\wvec}{\mathbf w}\) \(\newcommand{\xvec}{\mathbf x}\) \(\newcommand{\yvec}{\mathbf y}\) \(\newcommand{\zvec}{\mathbf z}\) \(\newcommand{\rvec}{\mathbf r}\) \(\newcommand{\mvec}{\mathbf m}\) \(\newcommand{\zerovec}{\mathbf 0}\) \(\newcommand{\onevec}{\mathbf 1}\) \(\newcommand{\real}{\mathbb R}\) \(\newcommand{\twovec}[2]{\left[\begin{array}{r}#1 \\ #2 \end{array}\right]}\) \(\newcommand{\ctwovec}[2]{\left[\begin{array}{c}#1 \\ #2 \end{array}\right]}\) \(\newcommand{\threevec}[3]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \end{array}\right]}\) \(\newcommand{\cthreevec}[3]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \end{array}\right]}\) \(\newcommand{\fourvec}[4]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \\ #4 \end{array}\right]}\) \(\newcommand{\cfourvec}[4]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \\ #4 \end{array}\right]}\) \(\newcommand{\fivevec}[5]{\left[\begin{array}{r}#1 \\ #2 \\ #3 \\ #4 \\ #5 \\ \end{array}\right]}\) \(\newcommand{\cfivevec}[5]{\left[\begin{array}{c}#1 \\ #2 \\ #3 \\ #4 \\ #5 \\ \end{array}\right]}\) \(\newcommand{\mattwo}[4]{\left[\begin{array}{rr}#1 \amp #2 \\ #3 \amp #4 \\ \end{array}\right]}\) \(\newcommand{\laspan}[1]{\text{Span}\{#1\}}\) \(\newcommand{\bcal}{\cal B}\) \(\newcommand{\ccal}{\cal C}\) \(\newcommand{\scal}{\cal S}\) \(\newcommand{\wcal}{\cal W}\) \(\newcommand{\ecal}{\cal E}\) \(\newcommand{\coords}[2]{\left\{#1\right\}_{#2}}\) \(\newcommand{\gray}[1]{\color{gray}{#1}}\) \(\newcommand{\lgray}[1]{\color{lightgray}{#1}}\) \(\newcommand{\rank}{\operatorname{rank}}\) \(\newcommand{\row}{\text{Row}}\) \(\newcommand{\col}{\text{Col}}\) \(\renewcommand{\row}{\text{Row}}\) \(\newcommand{\nul}{\text{Nul}}\) \(\newcommand{\var}{\text{Var}}\) \(\newcommand{\corr}{\text{corr}}\) \(\newcommand{\len}[1]{\left|#1\right|}\) \(\newcommand{\bbar}{\overline{\bvec}}\) \(\newcommand{\bhat}{\widehat{\bvec}}\) \(\newcommand{\bperp}{\bvec^\perp}\) \(\newcommand{\xhat}{\widehat{\xvec}}\) \(\newcommand{\vhat}{\widehat{\vvec}}\) \(\newcommand{\uhat}{\widehat{\uvec}}\) \(\newcommand{\what}{\widehat{\wvec}}\) \(\newcommand{\Sighat}{\widehat{\Sigma}}\) \(\newcommand{\lt}{<}\) \(\newcommand{\gt}{>}\) \(\newcommand{\amp}{&}\) \(\definecolor{fillinmathshade}{gray}{0.9}\)- Identify the major classes of hormones on the basis of chemical structure.
- Know the function of the common hormones.
Glands of the Endocrine System
The endocrine system is a system of glands called endocrine glands that release chemical messenger molecules into the bloodstream. The messenger molecules of the endocrine system are called endocrine hormones. The major glands of the endocrine system are shown in Figure \(\PageIndex{1}\). The major hormones of the human body and their effects are listed in Table \(\PageIndex{1}\).
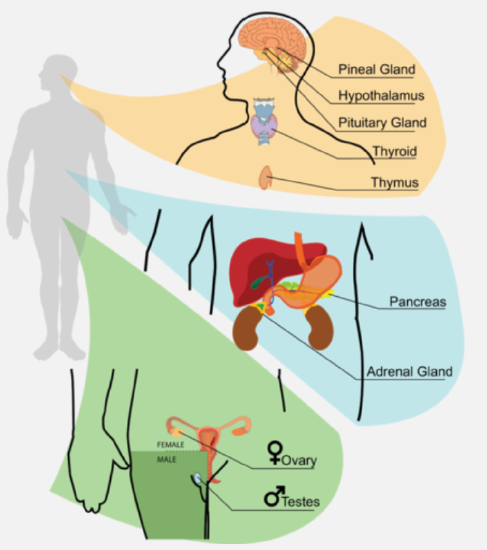
Although a given hormone may travel throughout the body in the bloodstream, it will affect the activity only of its target cells; that is, cells with receptors for that particular hormone. Once the hormone binds to the receptor, a chain of events is initiated that leads to the target cell’s response. Hormones play a critical role in the regulation of physiological processes because of the target cell responses they regulate. These responses contribute to human reproduction, growth and development of body tissues, metabolism, fluid, and electrolyte balance, sleep, and many other body functions. The major hormones of the human body and their effects are identified in Table \(\PageIndex{1}\).
| Endocrine gland | Associated hormones | Chemical class | Effect |
|---|---|---|---|
| Pituitary | Growth hormone (GH) | Protein | Promotes growth of body tissues |
| Prolactin (PRL) | Peptide | Promotes milk production | |
| Thyroid-stimulating hormone (TSH) | Glycoprotein | Stimulates thyroid hormone release | |
| Adrenocorticotropic hormone (ACTH) | Peptide | Stimulates hormone release by adrenal cortex | |
| Follicle-stimulating hormone (FSH) | Glycoprotein | Stimulates gamete production | |
| Luteinizing hormone (LH) | Glycoprotein | Stimulates androgen production by gonads | |
| Antidiuretic hormone (ADH) | Peptide | Stimulates water reabsorption by kidneys | |
| Oxytocin | Peptide | Stimulates uterine contractions during childbirth | |
| Thyroid | Thyroxine (T4), triiodothyronine (T3) | Amine | Stimulate basal metabolic rate |
| Calcitonin | Peptide | Reduces blood Ca2+ levels | |
| Parathyroid | Parathyroid hormone (PTH) | Peptide | Increases blood Ca2+ levels |
| Adrenal (cortex) | Aldosterone | Steroid | Increases blood Na+ levels |
| Cortisol, corticosterone, cortisone | Steroid | Increase blood glucose levels | |
| Adrenal (medulla) | Epinephrine, norepinephrine | Amine | Stimulate fight-or-flight response |
| Pineal | Melatonin | Amine | Regulates sleep cycles |
| Pancreas | Insulin | Protein | Reduces blood glucose levels |
| Glucagon | Protein | Increases blood glucose levels | |
| Testes | Testosterone | Steroid | Stimulates development of male secondary sex characteristics and sperm production |
| Ovaries | Estrogens and progesterone | Steroid | Stimulate development of female secondary sex characteristics and prepare the body for childbirth |
Types of Hormones
The hormones of the human body can be divided into two major groups on the basis of their chemical structure. Hormones derived from amino acids include amines, peptides, and proteins. Those derived from lipids include steroids (Figure \(\PageIndex{1}\)). These chemical groups affect a hormone’s distribution, the type of receptors it binds to, and other aspects of its function.
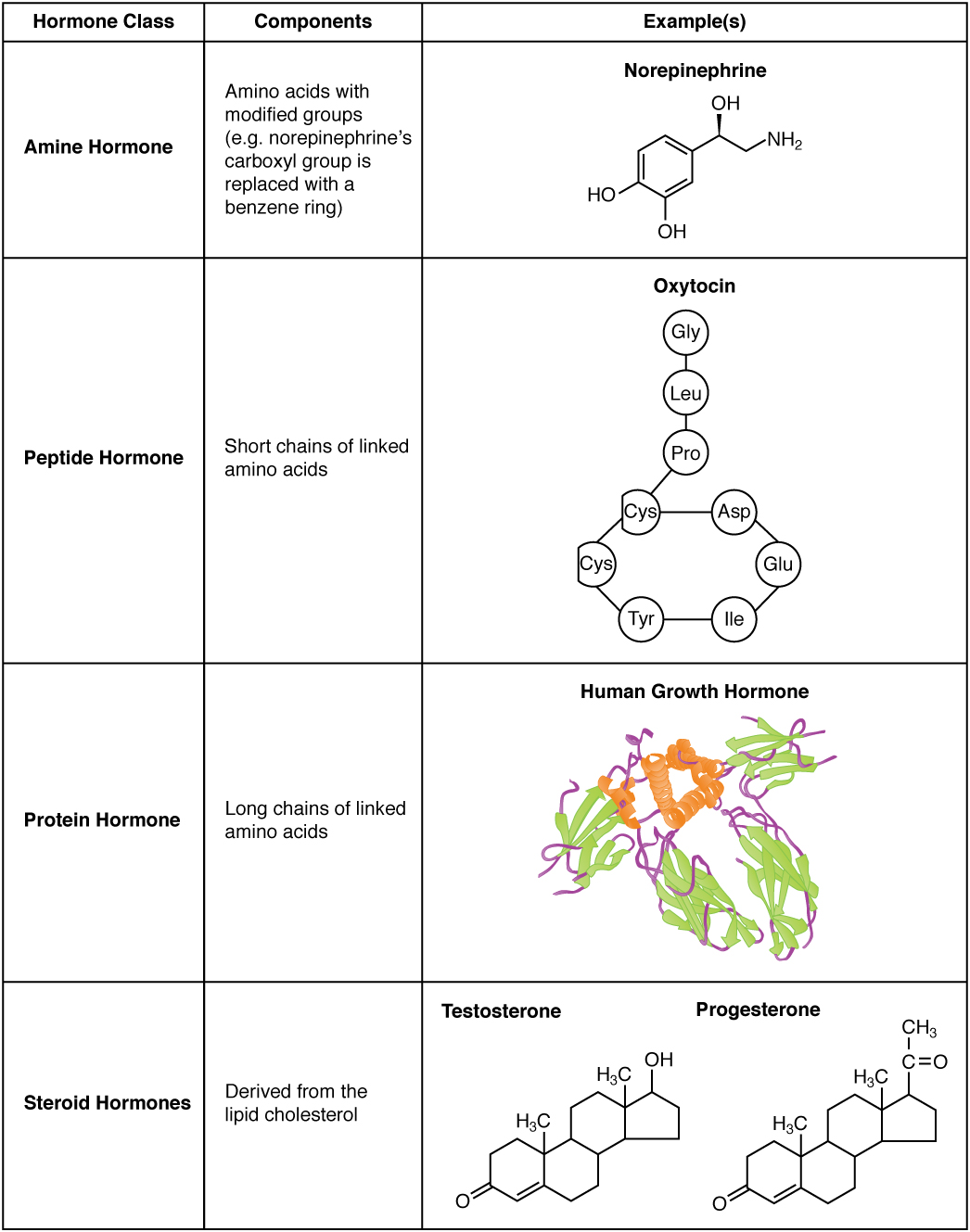
Amine Hormones
Hormones derived from the modification of amino acids are referred to as amine hormones. Typically, the original structure of the amino acid is modified such that a –COOH, or carboxyl, group is removed, whereas the −NH3+−NH3+, or amine, group remains.
Amine hormones are synthesized from the amino acids tryptophan or tyrosine. An example of a hormone derived from tryptophan is melatonin, which is secreted by the pineal gland and helps regulate circadian rhythm. Tyrosine derivatives include the metabolism-regulating thyroid hormones, as well as the catecholamines, such as epinephrine, norepinephrine, and dopamine. Epinephrine and norepinephrine are secreted by the adrenal medulla and play a role in the fight-or-flight response, whereas dopamine is secreted by the hypothalamus and inhibits the release of certain anterior pituitary hormones.
Peptide and Protein Hormones
Whereas the amine hormones are derived from a single amino acid, peptide and protein hormones consist of multiple amino acids that link to form an amino acid chain. Peptide hormones consist of short chains of amino acids, whereas protein hormones are longer polypeptides. Both types are synthesized like other body proteins: DNA is transcribed into mRNA, which is translated into an amino acid chain.
Examples of peptide hormones include antidiuretic hormone (ADH), a pituitary hormone important in fluid balance, and atrial-natriuretic peptide, which is produced by the heart and helps to decrease blood pressure. Some examples of protein hormones include growth hormone, which is produced by the pituitary gland, and follicle-stimulating hormone (FSH), which has an attached carbohydrate group and is thus classified as a glycoprotein. FSH helps stimulate the maturation of eggs in the ovaries and sperm in the testes.
Steroid Hormones
Hormones are chemical messengers that are released in one tissue and transported through the circulatory system to one or more other tissues. One group of hormones is known as steroid hormones because these hormones are synthesized from cholesterol, which is also a steroid. There are two main groups of steroid hormones: adrenocortical hormones and sex hormones.
Adrenocortical hormones
The adrenocortical hormones, such as aldosterone and cortisol (Table \(\PageIndex{1}\)), are produced by the adrenal gland, which is located adjacent to each kidney. Aldosterone acts on most cells in the body, but it is particularly effective at enhancing the rate of reabsorption of sodium ions in the kidney tubules and increasing the secretion of potassium ions and/or hydrogen ions by the tubules. Because the concentration of sodium ions is the major factor influencing water retention in tissues, aldosterone promotes water retention and reduces urine output. Cortisol regulates several key metabolic reactions (for example, increasing glucose production and mobilizing fatty acids and amino acids). It also inhibits the inflammatory response of tissue to injury or stress. Cortisol and its analogs are therefore used pharmacologically as immunosuppressants after transplant operations and in the treatment of severe skin allergies and autoimmune diseases, such as rheumatoid arthritis.
| Hormone | Effect |
|---|---|
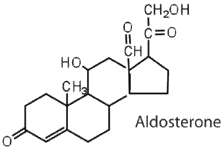 |
regulates salt metabolism; stimulates kidneys to retain sodium and excrete potassium |
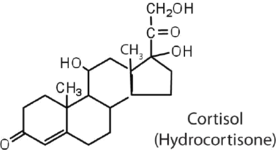 |
stimulates the conversion of proteins to carbohydrates |
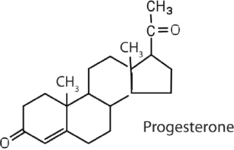 |
regulates the menstrual cycle; maintains pregnancy |
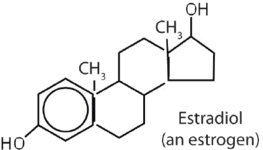 |
stimulates female sex characteristics; regulates changes during the menstrual cycle |
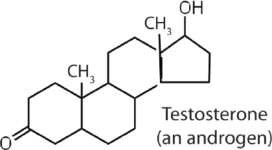 |
stimulates and maintains male sex characteristics |
Sex Hormones
The sex hormones are a class of steroid hormones secreted by the gonads (ovaries or testes), the placenta, and the adrenal glands. Testosterone and androstenedione are the primary male sex hormones, or androgens, controlling the primary sexual characteristics of males, or the development of the male genital organs and the continuous production of sperm. Androgens are also responsible for the development of secondary male characteristics, such as facial hair, deep voice, and muscle strength. Two kinds of sex hormones are of particular importance in females: progesterone, which prepares the uterus for pregnancy and prevents the further release of eggs from the ovaries during pregnancy, and the estrogens, which are mainly responsible for the development of female secondary sexual characteristics, such as breast development and increased deposition of fat tissue in the breasts, the buttocks, and the thighs. Both males and females produce androgens and estrogens, differing in the amounts of secreted hormones rather than in the presence or absence of one or the other.
Sex hormones, both natural and synthetic, are sometimes used therapeutically. For example, a woman who has had her ovaries removed may be given female hormones to compensate. Some of the earliest chemical compounds employed in cancer chemotherapy were sex hormones. For example, estrogens are one treatment option for prostate cancer because they block the release and activity of testosterone. Testosterone enhances prostate cancer growth. Sex hormones are also administered in preparation for sex-change operations, to promote the development of the proper secondary sexual characteristics. Oral contraceptives are synthetic derivatives of the female sex hormones; they work by preventing ovulation.
Chemistry and Social Revolution: The Pill
Hormonal contraception methods prevent pregnancy by interfering with ovulation, fertilization, and/or implantation of the fertilized egg.
Oral contraceptives—combined pill (“The pill”)
The pill contains the hormones estrogen and progestin. It is taken daily to keep the ovaries from releasing an egg. The pill also causes changes in the lining of the uterus and the cervical mucus to keep the sperm from joining the egg.
Some women prefer the “extended cycle” pills. These have 12 weeks of pills that contain hormones (active) and 1 week of pills that don’t contain hormones (inactive). While taking extended cycle pills, women only have their period three to four times a year.
Many types of oral contraceptives are available. Talk with your doctor about which is best for you.
Your doctor may advise you not to take the pill if you:
- Are older than 35 and smoke
- Have a history of blood clots
- Have a history of breast, liver, or endometrial cancer
Antibiotics may reduce how well the pill works in some women. Talk to your doctor about a backup method of birth control if you need to take antibiotics.
Women should wait three weeks after giving birth to begin using birth control that contains both estrogen and progestin. These methods increase the risk of dangerous blood clots that could form after giving birth. Women who delivered by cesarean section or have other risk factors for blood clots, such as obesity, history of blood clots, smoking, or preeclampsia, should wait six weeks.
The patch
Also called by its brand name, Ortho Evra, this skin patch is worn on the lower abdomen, buttocks, outer arm, or upper body. It releases the hormones progestin and estrogen into the bloodstream to stop the ovaries from releasing eggs in most women. It also thickens the cervical mucus, which keeps the sperm from joining with the egg. You put on a new patch once a week for 3 weeks. You don’t use a patch the fourth week in order to have a period.
Women should wait three weeks after giving birth to begin using birth control that contains both estrogen and progestin. These methods increase the risk of dangerous blood clots that could form after giving birth. Women who delivered by cesarean section or have other risk factors for blood clots, such as obesity, history of blood clots, smoking, or preeclampsia, should wait six weeks.
Shot/injection
The birth control shot often is called by its brand name Depo-Provera. With this method you get injections, or shots, of the hormone progestin in the buttocks or arm every 3 months. A new type is injected under the skin. The birth control shot stops the ovaries from releasing an egg in most women. It also causes changes in the cervix that keep the sperm from joining with the egg.
Vaginal ring
This is a thin, flexible ring that releases the hormones progestin and estrogen. It works by stopping the ovaries from releasing eggs. It also thickens the cervical mucus, which keeps the sperm from joining the egg.
It is commonly called NuvaRing, its brand name. You squeeze the ring between your thumb and index finger and insert it into your vagina. You wear the ring for 3 weeks, take it out for the week that you have your period, and then put in a new ring.
Women should wait three weeks after giving birth to begin using birth control that contains both estrogen and progestin. These methods increase the risk of dangerous blood clots that could form after giving birth. Women who delivered by cesarean section or have other risk factors for blood clots, such as obesity, history of blood clots, smoking, or preeclampsia, should wait six weeks.
Implantable devices
These devices are inserted into the body and left in place for a few years.
Implantable rod
This is a matchstick-size, flexible rod that is put under the skin of the upper arm. It is often called by its brand name, Implanon. The rod releases a progestin, which causes changes in the lining of the uterus and the cervical mucus to keep the sperm from joining an egg. Less often, it stops the ovaries from releasing eggs. It is effective for up to 3 years.
Intrauterine devices or IUDs
- Hormonal IUD The hormonal IUD goes by the brand name Mirena. It is sometimes called an intrauterine system, or IUS. It releases progestin into the uterus, which keeps the ovaries from releasing an egg and causes the cervical mucus to thicken so sperm can’t reach the egg. It also affects the ability of a fertilized egg to successfully implant in the uterus. A doctor needs to put in a hormonal IUD. It can stay in your uterus for up to 5 years.
Emergency Contraceptives
Emergency contraceptives are used if a woman’s primary method of birth control fails. It should not be used as a regular method of birth control. The emergency contraceptive, Plan B One-Step or Next Step is also called the “morning after pill.”
Emergency contraception keeps a woman from getting pregnant when she has had unprotected vaginal intercourse. “Unprotected” can mean that no method of birth control was used. It can also mean that a birth control method was used but it was used incorrectly, or did not work (like a condom breaking). Or, a woman may have forgotten to take her birth control pills. She also may have been abused or forced to have sex. These are just some of the reasons women may need emergency contraception.
Emergency contraception can be taken as a single pill treatment or in two doses. A single dose treatment works as well as two doses and does not have more side effects. It works by stopping the ovaries from releasing an egg or keeping the sperm from joining with the egg. For the best chances for it to work, take the pill as soon as possible after unprotected sex. It should be taken within 72 hours after having unprotected sex.
A single-pill dose or two-pill dose of emergency contraception is available over-the-counter (OTC) for women ages 17 and older.
Summary
- A hormone is any member of a class of signaling molecules, produced by glands in multicellular organisms to regulate physiology and behavior.
- The hormones of the human body can be divided into two major groups on the basis of their chemical structure. Hormones derived from amino acids include amines, peptides, and proteins. Those derived from lipids include steroids.
- The two main groups of steroid hormones: adrenocortical hormones and sex hormones.
- Hormonal contraception methods prevent pregnancy by interfering with ovulation, fertilization, and/or implantation of the fertilized egg.
- Emergency contraceptives are used if a woman’s primary method of birth control fails.
Contributors
- Libretext: Anatomy and Physiology (OpenStax)
- Libretext: Human Biology (Wakim and Grewal)
- Libretexts: Survey of Chemistry (Cannon)
- Libretexts: The Basics of GOB Chemistry (Ball et.al.)
- Libretexts: Contemporary Health Issues (Lumen)
- Wikipedia

