1.2: A Drug's Life
- Page ID
- 211464
Antibiotic Cholesterol Bacterium Death Gene Cholesterol Cyclooxygenase abiotic transformation α-cleavage work
How does aspirin zap a headache? What happens after you rub some cortisone cream on a patch of poison ivy-induced rash on your arm? How do decongestant medicines such as Sudafed® dry up your nasal passages when you have a cold? As medicines find their way to their "job sites" in the body, hundreds of things happen along the way. One action triggers another, and medicines work to either mask a symptom, like a stuffy nose, or fix a problem, like a bacterial infection.
A Model for Success
Turning a molecule into a good medicine is neither easy nor cheap. The Center for the Study of Drug Development at Tufts University in Boston estimates that it takes over $800 million and a dozen years to sift a few promising drugs from about 5,000 failures. Of this small handful of candidate drugs, only one will survive the rigors of clinical testing and end up on pharmacy shelves.
That's a huge investment for what may seem a very small gain and, n part, it explains the high cost of many prescription drugs. Sometimes, problems do not show up until after a drug reaches the market and many people begin taking the drug routinely. These problems range from irritating side effects, such as dry mouth or drowsiness, to life-threatening problems like serious bleeding or blood clots. The outlook might be brighter if pharmaceutical scientists could do a better job of predicting how potential drugs will act in the body (a science called pharmacodynamics), as well as what side effects the drugs might cause.
One approach that can help is computer modeling of a drug's properties. Computer modeling can help scientists at pharmaceutical and biotechnology companies filter out, and abandon early on, any candidate drugs that are likely to behave badly in the body. This can save significant amounts of time and money.
Computer software can examine the atom-by-atom structure of a molecule and determine how durable the chemical is likely to be inside a body's various chemical neighborhoods. Will the molecule break down easily? How well will the small intestines take it in? Does it dissolve easily in the watery environment of the fluids that course through the human body? Will the drug be able to penetrate the blood-brain barrier? Computer tools not only drive up the success rate for finding candidate drugs, they can also lead to the development of better medicines with fewer safety concerns.


A drug's life in the body. Medicines taken by mouth (oral) pass through the liver before they are absorbed into the bloodstream. Other forms of drug administration bypass the liver, entering the blood directly.
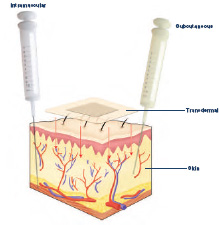
Drugs enter different layers of skin via intramuscular, subcutaneous, or transdermal delivery methods.
Scientists have names for the four basic stages of a medicine's life in the body: absorption, distribution, metabolism, and excretion. The entire process is sometimes abbreviated ADME. The first stage is absorption. Medicines can enter the body in many different ways, and they are absorbed when they travel from the site of administration into the body's circulation. A few of the most common ways to administer drugs are oral (swallowing an aspirin tablet), intramuscular (getting a flu shot in an arm muscle), subcutaneous (injecting insulin just under the skin), intravenous (receiving chemotherapy through a vein), or transdermal (wearing a skin patch), A drug faces its biggest hurdles during absorption. Medicines taken by mouth are shuttled via a special blood vessel leading from the digestive tract to the liver, where a large amount may be destroyed by metabolic enzymes in the so-called "first-pass effect." Other routes of drug administration bypass the liver, entering the bloodstream directly or via the skin or lungs.
Once a drug gets absorbed, the next stage is distribution. Most often, the bloodstream carries medicines throughout the body. During this step, side effects can occur when a drug has an effect in an organ other than the target organ. For a pain reliever, the target organ might be a sore muscle in the leg; irritation of the stomach could be a side effect. Many factors influence distribution, such as the presence of protein and fat molecules in the blood that can put drug molecules out of commission by grabbing onto them.
Drugs destined for the central nervous system (the brain and spinal cord) face an enormous hurdle: a nearly impenetrable barricade called the blood-brain barrier. This blockade is built from a tightly woven mesh of capillaries cemented together to protect the brain from potentially dangerous substances such as poisons or viruses. Yet pharmacologists have devised various ways to sneak some drugs past this barrier.
After a medicine has been distributed throughout the body and has done its job, the drug is broken down, or metabolized. The breaking down of a drug molecule usually involves two steps that take place mostly in the body's chemical processing plant, the liver. The liver is a site of continuous and frenzied, yet carefully controlled, activity. Everything that enters the bloodstream—whether swallowed, injected, inhaled, absorbed through the skin, or produced by the body itself—is carried to this largest internal organ. There, substances are chemically pummeled, twisted, cut apart, stuck together, and transformed.
Medicines and Your Genes

How you respond to a drug may be quite different from how your neighbor does. Why is that? Despite the fact that you might be about the same age and size, you probably eat different foods, get different amounts of exercise, and have different medical histories. But your genes, which are different from those of anyone else in the world, are really what make you unique. In part, your genes give you many obvious things, such as your looks, your mannerisms, and other characteristics that make you who you are. Your genes can also affect how you respond to the medicines you take. Your genetic code instructs your body how to make hundreds of thousands of different molecules called proteins. Some proteins determine hair color, and some of them are enzymes that process, or metabolize, food or medicines. Slightly different, but normal, variations in the human genetic code can yield proteins that work better or worse when they are metabolizing many different types of drugs and other substances. Scientists use the term pharmacogenetics to describe research on the link between genes and drug response.
One important group of proteins whose genetic code varies widely among people are "sulfation" enzymes, which perform chemical reactions in your body to make molecules more water-soluble, so they can be quickly excreted in the urine. Sulfation enzymes metabolize many drugs, but they also work on natural body molecules, such as estrogen. Differences in the genetic code for sulfation enzymes can significantly alter blood levels of the many different kinds of substances metabolized by these enzymes. The same genetic differences may also put some people at risk for developing certain types of cancers whose growth is fueled by hormones like estrogen.
Pharmacogeneticist Rebecca Blanchard of Fox Chase Cancer Center in Philadelphia has discovered that people of different ethnic backgrounds have slightly different "spellings" of the genes that make sulfation enzymes. Lab tests revealed that sulfation enzymes manufactured from genes with different spellings metabolize drugs and estrogens at different rates. Blanchard and her coworkers are planning to work with scientists developing new drugs to include pharmacognetic testing in the early phases of screening new medicines.
The biotransformations that take place in the liver are performed by the body's busiest proteins, its enzymes. Every one of your cells has a variety of enzymes, drawn from a repertoire of hundreds of thousands. Each enzyme specializes in a particular job. Some break molecules apart, while others link small molecules into long chains. With drugs, the first step is usually to make the substance easier to get rid of in urine.
Many of the products of enzymatic break-down, which are called metabolites, are less chemically active than the original molecule. For this reason, scientists refer to the liver as a "detoxifying" organ. Occasionally, however, drug metabolites can have chemical activities of their own—sometimes as powerful as those of the original drug. When prescribing certain drugs, doctors must take into account these added effects. Once liver enzymes are finished working on a medicine, the now-inactive drug undergoes the final stage of its time in the body, excretion, as it exits via the urine or feces.
Perfect Timing
Pharmacokinetics is an aspect of pharmacology that deals with the absorption, distribution, and excretion of drugs. Because they are following drug actions in the body, researchers who specialize in pharmacokinetics must also pay attention to an additional dimension: time.
Pharmacokinetics research uses the tools of mathematics. Although sophisticated imaging methods can help track medicines as they travel through the body, scientists usually cannot actually see where a drug is going. To compensate, they often use mathematical models and precise measures of body fluids, such as blood and urine, to determine where a drug goes and how much of the drug or a break-down product remains after the body processes it. Other sentinels, such as blood levels of liver enzymes, can help predict how much of a drug is going to be absorbed.
Studying pharmacokinetics also uses chemistry, since the interactions between drug and body molecules are really just a series of chemical reactions. Understanding the chemical encounters between drugs and biological environments, such as the bloodstream and the oily surfaces of cells, is necessary to predict how much of a drug will be taken in by the body. This concept, broadly termed bioavailability, is a critical feature that chemists and pharmaceutical scientists keep in mind when designing and packaging medicines. No matter how well a drug works in a laboratory simulation, the drug is not useful if it can't make it to its site of action.

